BUILDING BETTER BREASTS
Stem Cell Techniques in Breast Augmentation
Why Bigger Breasts?
Tissue Engineering
Stem Cells & Breasts
Future Directions
References
Future Directions
Making them bigger: currently the maximum volume increase achieved by cell-assisted lipotransfer is 100-200ml, or approximately 2-3 cup sizes [6]. While this may be acceptable for reconstructive surgery and even the average cosmetic surgery, some people want or need more. It would be impractical, for example, to give a women who naturally had large breasts but lost one due to a mastectomy after breast cancer, the cell-assisted lipotransfer treatment. 100-200ml may not be enough to restore the breast to match its counterpart and therefore would certainly not alleviate the problem of asymmetry.
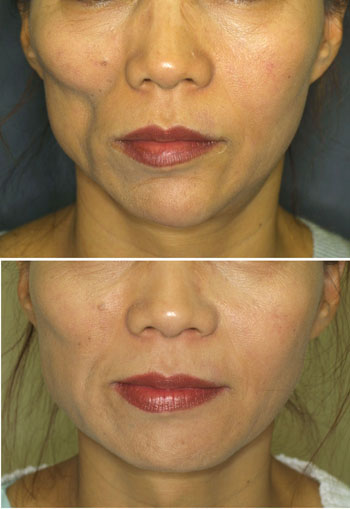 Figure 9: Cell-assisted lipotransfer for facial lipoatrophy |
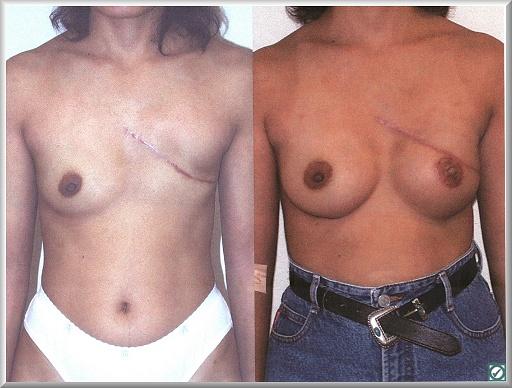 Figure 11: Unfortunatey, after a devastating mastectomy cell-assisted lipotransfer may not provide needed volume
|
Increasing the size of the breast is not the only therapy that can be realized using cell-assisted lipotransfer. Any reconstructive or cosmetic surgery that involves the transplant of fat cells can be adapted to take advantage of cell-assisted lipotransfer and subsequently improved upon. In addition to breast augmentation, cell-assisted lipotransfer has been used in facial lipoatrophy to restore the face [8]. This therapy uses the exact same principle as mentioned previously but applies it to the face where, as shown in figure 9, the indenation appears. Fortunately the therapy is effective (at least in trials thus far) and the woman shown seems to have recovered nicely.
Stem cells as a whole have a bright future in the field of tissue engineering. Reconstructive surgery is certainly not the only option for stem cells and although a comprehensive review of their potential and behavior is well beyond the scope of this site, it is possible to say that eventually it may be possible to re-grow nearly any organ for transplantation. It may even be possible to regenerate organs in situ in the future, eliminating the need for organ transplantation.
Virtually every organ in the human body has been grown, to some capacity in the laboratory and scientists are advancing rapidly in the area of organ replacement. The human bladder has been not only grown in lab, but actually transplanted [9]. In the referenced study by Atala et al all of the bladders received by the patients were successfully transplanted and integtrated into the host tissue, and five year follow-up showed that the patients were not experiencing complications. The amazing and promising fact of this study is that autologous tissue, just like in cell-assisted lipotransfer, was used to grow the organ, which made immune rejection an impossibility (something that would have to be considered in a transplant from an allogenic source (another human).