

Introduction

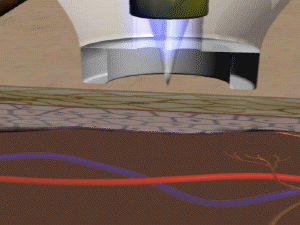
Non-invasive optical detection methods have recently become viable alternatives to monitoring blood glucose levels. Spectrophotometry is an established method for the quantification of solutes in liquids. It is based on solute specific absorption bands in the visible (VIS), near infra-red (NIR) or mid infra-red (MIR) spectral range. Quantification of the solutes is possible by determination of light attenuation caused by absorption at a single wavelength when taking the light path length (i. e. the cuvette thickness) into account. The solution has to be clear, as light scattering would result in an additional attenuation of light.
Quantification of a single solute in a complex mixture of substances is possible using various wavelengths and requires complex mathematical procedures like multivariate calibration. Today the ex vivo quantification of glucose in complex matrices like plasma, serum or whole blood is feasible by using high performance spectroscopic equipment in combination with sophisticated mathematical calibration procedures. MIR radiation is particularly appropriate for such measurements because glucose specific absorption bands are prominent in this frequency range. Thus, it can be expected that it is also possible to use spectrophotometric approaches to measure glucose non-invasively in the skin. Water, however, as the main tissue constituent and many other components of skin, absorb MIR radiation very effectively. Hence, the in-vivo penetration depth of MIR-light in skin is low [15]. In contrast, light in the NIR and VIS region penetrates to deeper blood perfused skin layers potentially allowing for glucose monitoring (ªoptical windowº) and glucose exhibits no specific absorption properties in this frequency range. If tissue thickness is low, transmission spectra can be recorded. Otherwise only diffusely reflected light intensity has to be used. The current status of blood glucose monitoring in human skin by near infra-red absorption measurements using different spectrophotometric methods has been reviewed recently.2